Integrative Medicine Man
The hiccups wouldn’t stop. It was August of 1996, and an elderly stroke victim lay dying in his home in the small town of Driggs, Idaho. But he could have no rest. He was stricken with a relentless case of hiccups, robbing him of comfort.
The episode gave David Rakel, the man’s physician and neighbor, a memorable lesson in the importance of watching, listening, and heeding the desires of his patients. Drugs, the main weapon in Rakel’s medical arsenal, made the dying man groggy and unaware, and still the hiccups continued. Family members suggested acupuncture.
Like many conventional, or allopathic, Western physicians, Rakel was skeptical. But he figured acupuncture would do no harm. “I humored them. I said, ‘Sure. Why not?’ ” It worked. The acupuncturist came. The hiccups went away without sedation. “He was able to die with loving family around him and a sense of peace. It was a beautiful death,” says Rakel, now a UW-Madison professor of family medicine. “If I had given him more drugs, he would have been lethargic. He would not have been present with his loved ones.”
The incident started Rakel on a path that would lead to his founding the university’s integrative medicine program in 2001.
That journey to the Midwest began in Driggs, nestled between the Tetons and the Big Hole Mountains and just over the pass from Jackson Hole, Wyoming, where he first hung out his shingle as a rural family practice physician. It was there that he began to shed his skepticism about acupuncture, herbal supplements, guided imagery, and a host of healing techniques that he believes medicine can add seamlessly to the mix of traditional Western options.

David Rakel started the Integrative Medicine Research Park Clinic, which offers services such as meditation classes for stress reduction. Since arriving on campus, Rakel has taught a variety of integrative medicine techniques to both students and fellow physicians.
The Soul of Medicine
In 1999, Rakel decided to learn as much as he could about integrative medicine. He left Idaho for a two-year fellowship at the University of Arizona in Tucson. There, surrounded by desert peace and beauty and influenced by a steady stream of superstars in the field of healing arts and science, he took lessons in the heart, soul, art, and spirit of medicine.
His calling was to bring those lessons back to the broader world of American health care and help integrate them with the best that conventional medicine has to offer. He spent those fellowship years learning how integrative medicine rests on four pillars of health promotion: social, psychological, physical, and environmental.
Once considered on the fringes of health science, integrative medicine has gotten a boost from technology such as functional magnetic resonance imaging, which shows pathways between mind and body, and from research that backs up connections between nutrition, physical activity, and good health.
It’s been a decade since Rakel’s training at the Arizona Center for Integrative Medicine, and he’s just been approved for tenure at the UW. For John Frey, professor in the Department of Family Medicine and the man who hired Rakel in 2001, Rakel’s interest in integrative medicine has been a bonus. “What attracted me about him was that he’s a talented doctor with a wonderful perspective on patient and family care,” says Frey. “The integrative medicine program was something I didn’t know much about.”
Frey was key to getting Rakel to come to Wisconsin. But so was an unconventional decision-making method. Following his fellowship, Rakel weighed teaching offers in Colorado and Wisconsin. Torn by what he saw as two excellent options, he turned to guided imagery. In his mind, he went flying on the wings of an eagle.
Based on the concept that the body and mind are connected, guided imagery is a way of employing all the senses to help steer imagination. The body can respond as though what’s being imagined is a real event. A classic example is to imagine a lemon — think of peeling it, smelling it, squirting it in your mouth. Do your lips purse up in response?
In medicine, guided imagery can be used to control pain and stress. Cancer patients, for example, may be encouraged to imagine tiny healthy cells overpowering destructive cancer cells in their bodies. While the American Cancer Society says there’s no proof that guided imagery influences the progress of cancer, the ACS Web site does cite evidence that the technique can reduce stress, anxiety, and pain and lessen some of the side effects of chemotherapy, such as nausea and vomiting.
As Rakel imagined a golden eagle, he says, “he picked me up by the collar and we went flying.” And knowing how that must sound, Rakel hurriedly assures with a laugh: “No hallucinogens. All with our own bodies. I looked down and there were lakes and oak trees.” No snow-topped mountains. No aspens. He was looking down at the lakes and forests of the upper Midwest, not at the Rocky Mountains. “So we came to Wisconsin,” he says.
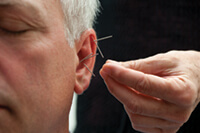
Another service offered by the integrative medicine clinics is acupuncture, which is designed to stimulate the natural healing processes of the body and is used to treat problems such as stress, nausea, pain, and other conditions.
Mentoring Students and Patients
At the UW, Rakel began teaching integrative medicine techniques to students, as well as fellow physicians. “He’s been able to attract a substantial number of young clinicians who agree there are a variety of different approaches to care,” says Frey. “He’s developed a very talented group of young family doctors, and was instrumental in getting a fellowship program going.”
In 2002, Luke Fortney ’98, MD’03, now an assistant professor in the family medicine program, was the first of Rakel’s students in a month-long elective rotation in integrative medicine. “Dr. Rakel has been a mentor from that point forward,” Fortney says. In addition to editing the field’s key textbook, Integrative Medicine, Rakel’s work today centers on teaching and caring for patients at the Integrative Medicine Odana Atrium Clinic on Madison’s west side and the Integrative Medicine Research Park Clinic. He also started the integrative medicine clinic at the Comprehensive Cancer Center at the UW Hospital.
Each facility offers therapies such as massage and acupuncture; the Research Park clinic also provides health psychology, Feldenkrais (movement therapy), healing touch, mindfulness stress reduction, yoga, and tai chi.
Patients are taught to meditate to reduce stress and encouraged to eat a diet rich in fruits, vegetables, whole grains, nuts, soy, olive oil, cold-water fish, and dark-colored berries for heart health. Part of their prescription for good health will surely be to exercise and get moderate sunshine to reduce depression. They might be told to try acupuncture for arthritis pain. And their spiritual beliefs will be considered as individual health plans are developed. Often, patients who come to the clinics are facing difficult chronic diseases and complicated tangles of symptoms.
For Lynette Peterson, Rakel has been a lifesaver. Now sixty-five, she has had multiple sclerosis, a disease that attacks the central nervous system, for thirty-five years. Symptoms can be mild or increasingly severe, but there is no cure. She found Rakel after her physician prescribed a chemotherapy regimen that left her with hair loss, sores on her lips and tongue, and loss of control of her bladder and bowels. “I told him I couldn’t take any more chemotherapy.
It was killing me,” she says. Rakel steered Peterson to acupuncture, changed some of her prescription medications, added dietary suggestions, and encouraged the use of fish oil, herbs, and regular exercise. It has taken more than a year, and hasn’t been a miraculous cure for Peterson, who remains in a wheelchair. But her symptoms have stabilized. “He’s got such a positive approach,” she says. “He knows he can’t cure everybody. But he also knows there are things he can do to make their lives easier.” She swims twice a week, remembering his advice: ‘Keep exercising, keep swimming. Think positive, think positive.’ ”
But changing an American’s lifestyle is difficult. Rakel is realistic, seeing change as a highly individual endeavor. A lifestyle prescription must, he has written, “be individualized based on the health, energy, resources, and personality of the patient.” “We really spend a lot of time listening,” Fortney says of those who practice integrative medicine. They listen for clues about what in patients’ lives might be contributing to ailments such as restless leg, acid reflux, or chronic pain, as well as what they might be willing to do to make changes.
Conventional medicine is part of integrated medicine. In fact, Frey says, without that mix, integrative medicine would get no respect. “If it becomes part of what doctors do in primary care, working with different healers as a team, then I think it has an important role,” says Frey.
Patients in integrative medicine, like any primary care patients, get flu shots, blood-pressure medications, or recommendations for surgery when their health calls for allopathic medicine. “I have no hesitation to use drugs,” Rakel says. “They’re often indicated and beneficial.” But all the while, patients are encouraged to look beyond a quick prescription-pad solution for what ails them, and to take as much control as they can over their well-being.
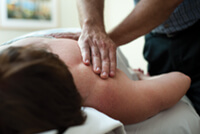
Massage therapists treat conditions such as back and neck pain, headaches, sports injuries, and stress. According to a clinic brochure, the staff focuses on less invasive therapies such as massage “to help remove barriers that may be blocking the body’s ability to heal.”
Ups and Downs
With fundamental changes to the nation’s health care delivery system recently passed into law, integrative medicine may well get increased attention. And it should, according to an article that Rakel co-authored with Wayne Jonas in a 2009 issue of Alternative Therapies.
“If the health reformers are looking to get the biggest ‘bang for their buck’ both in the prevention and management of chronic disease,” they wrote, “they need look no further than delivering [integrative medicine’s] four pillars [of social, psychological, physical, and environmental health].”
It’s not certain how integrative medicine will fare under the newly passed health reform law. But, according to the Integrated Health Care Policy Consortium, a coalition of conventional, alternative, and complementary health professionals, there are some positive signs. They include an emphasis on prevention, and on standards of evidence that will allow alternative therapies to be evaluated head-to-head with conventional therapies.
The hope is that as scientific studies find alternative therapies to be beneficial, insurers will cover them, just as they do a proven blood-pressure medication or an effective surgical procedure. Rakel says this doesn’t necessarily pan out, however, as there is now “good evidence for acupuncture,” and very few insurers cover it.
The discipline has had its ups and downs since Rakel’s training in integrative medicine began in Tucson. He was one of four fellows to study with Andrew Weil, a pioneer in a field that has changed names a few times as it has slowly earned grudging respect. The label alternative medicine has morphed into integrative medicine, via the terms “complementary” and “holistic.”
But by any other name, it means health care as opposed to disease care, an emphasis on wellness even as it deals with illness. And it is based on the same rigorous standards of evidence as any branch of medicine. “This is not belief without substance,” says Frey. “[Integrative medicine is] dedicated to pursuing the science behind [the discipline].”
Its practitioners are schooled in ways to hold on to their hearts and souls even as they master the intricacies of anatomy, physiology, biology, and psychology. They see their work as healing the whole patient, rather than being limited to specific body parts. When integrative medicine is hot, the universe responds with initiatives such as an office within the National Institutes of Health. When it’s not, funds are cut. “In my career, it’s gone up and down about three times,” says Rakel. “The financial incentives [that focus on rewarding the treatment of disease] always swing against it.”
Even as acceptance grows, there are setbacks. In 2009, physician Lucille Marchand saw her integrative medicine work at the UW oncology clinic go from full time to one day a week because of a funding reduction from the hospital. Fortunately, the Department of Family Medicine stepped in, providing resources to continue her work. The care she provides involves listening and talking, not performing high-income-yielding procedures. “Hospitals see integrative medicine as less necessary. If they’re going to survive, they feel they need to maximize interventions,” she says. “One oncologist said he didn’t believe in integrative medicine. Luckily, most oncologists and other cancer health professionals see the benefit.”
Rakel confirms that “the UW Hospital has been supportive of our program” and that an interdisciplinary UW Hospital Health and Healing Committee was started a few years ago for just that purpose. The American health care system, however, has always rewarded physicians skilled in invasive procedures more than those who listen to patients and talk them through healing. A heart surgeon, for example, earns an average of $515,000 a year, according to an Allied Physicians salary survey, while a family practice physician averages $135,000.
And primary care physicians, forced by the health care delivery system to spend as little as fifteen or twenty minutes with a patient, don’t have the time they need to get to the core of symptoms or to really influence the course of a chronic disease. The way payment incentives are set up through America’s insurance systems, a physician earns more for seeing four patients in an hour than for spending an entire hour with one patient. “[Practitioners] get good at seeing people quickly by just treating symptoms,” Rakel says. “If someone comes in with upper gastric pain, I can turn that off with Prilosec, and the patient leaves happy. But we miss out on what that symptom is trying to teach us, what it is that might be eating [the patient] up inside.”
An Ounce of Prevention
Contemporary American medicine focuses on diagnosis and treatment of existing disease. “We have a wonderful disease care system,” Rakel says. “We can reverse acute episodes of disease. But we haven’t paid enough attention to helping people avoid disease.”
Rakel is a staunch advocate for moving prevention and wellness from an afterthought to the core mission of health care. Study after study shows that he is on to something. In January 2010, the New England Journal of Medicine found compelling evidence that reducing salt intake would save lives and money.
A public health intervention designed to reduce salt consumption by 1,200 milligrams — or about two-thirds of a teaspoon — a day, could nearly cut in half the number of new cases of heart disease, stroke, and heart attack. In the process, it could save between $10 billion and $24 billion a year in health care costs. “This is a good example of how a low-cost intervention can result in dramatic effects on human health,” Rakel says.
But making it work for millions of people is profoundly difficult. “To understand how to implement a low-salt program, we have to understand how complex systems interact. We need to communicate a common goal to the food industry, school lunch programs, marketing personnel,” Rakel says. “We need to create financial incentives to make these changes. No one makes money by reducing salt in the diet.”
Like many lifestyle changes, reducing salt intake is so much easier said than done. A 2005 study in the Archives of Internal Medicine examined the top five health-producing behaviors: not smoking, getting adequate exercise, eating a healthy diet, managing stress, and using early disease detection tools such as mammograms and colonoscopies. The study found that only 2 to 4 percent of Americans engage in all of them.
Helping people change unhealthy lifestyles requires an investment in health care teams that will stand by patients as they try to change. Rakel is now working on just such an initiative to create patient-centered units — being recognized nationally in primary care as “medical homes” — that are composed of teams of treatment professionals. Generally these teams consist of doctors and nurses, but Rakel would also like to include nutritionists, exercise physiologists, health psychologists, social workers, and even spiritual guides working with individuals to help them stay healthy on their own terms. While a physician may lead the medical team, the workload is shared among various professionals, and the patient ends up getting more time devoted to health education, disease prevention, and chronic disease control.
The goal is to shift the health care system from its emphasis on reacting to a symptom or disease toward being more proactive. Rather than waiting for a person to develop diabetes, for example, and then rushing in with kidney dialysis or surgery for failing kidneys or limbs, Rakel hopes that developing these health teams will help with prevention. “These lessons are hard to learn,” he says. “But what if we had whole teams of professionals to help make those [lifestyle] changes? We need our health and political leadership to stress the importance of this.”
He continues to go back to lessons learned from the folks in the small Western town of Driggs, Idaho, with its 1,300 people and its fourteen-bed hospital. In a town that small, a doctor doesn’t wait until people come into the office to make observations about their well-being. “You see your patients at the grocery store and in church,” he says. “You develop insights into why they might be coming to see you with headaches.”
His initial skepticism has turned to enthusiasm, and then evolved into a true passion for practicing and teaching as one of the nation’s leaders in integrative medicine. Rakel knows that not everyone will buy the whole package, which could include flying with an imaginary golden eagle to help nail down a difficult decision. But offering options such as guided imagery, acupuncture, nutrition education, and lifestyle advice along with conventional medical options can help.
“You’ve got to read your audience,” he says, “meet them where they’re at, and maybe bring them to a new place of awareness.” Susan Brink is a freelance health writer based in Chicago. She has written for U.S. News & World Report and the LA Times and has published online for MSNBC.com and the Boston Globe.
Published in the Fall 2010 issue




Comments
Rebecca September 17, 2010
I have been a nurse(LPN)for the past 2 and 1/2 years at a clinic in St. Croix Falls WI. My desire to get into health care was prompted by my interest in alternative medicine. Understanding that there are not a lot of jobs in this field I turned to traditional medicine. Years prior to becoming a nurse I read and did research on a lot of diseases and how people have used alternative treatments to overcome their ailment. The main thing that I have learned is that anything is possible, and the power of the mind is incredible. It is the seat to the immune system and a healthy immune system is the cornerstone to all healing.
I recently approaced the CEO of this organization to see if he would be interested in starting an integrated medicine progam here. Not sure what would be needed to start other than my desire to truely help others. If you could give me some ideas as to how to get started in this field I would appreciate it. I also understand that I would need to get a doctor to oversee this venture as I am a LPN.
Thank you for your time,
Rebecca
Tim September 29, 2010
For shame, Wisconsin. You have made me embarrassed to be a UW alumnus.
There is no evidence to support the various treatments identified here, like acupuncture and healing touch, as offering anything beyond placebo. I honestly cannot understand how a serious institution like the UW can offer treatments that lack any scientific basis.
There is no such thing as “alternative” medicine. Medicine is a science. Its claims must therefore be supported by evidence, not anecdote. If someone has a theory about a course of treatment, it is subject to testing. If the tests prove that it works, and are replicated, this course of treatment becomes “medicine” (which is the same thing as “conventional medicine”).
For example, there is nothing “alternative” about the claim that there is a link between nutrition and physical activity, on the one hand, and good health. There is evidence to support these claims, and this evidence has been replicated in a number of tests. This claim should not be compared to claims that therapies like acupuncture and massage help “remove barriers” that “may be blocking the body’s ability to heal”. There is no evidence to support this.
Moreover, by linking such a program to a normally well-respected institution, you give credence to the claim that these treatments are a valid alternative to so-called conventional medicine. They are not. People have died, and will continue to die, by opting for “alternative” approaches instead of real medicine.
Let’s apply the University’s resources to treatments that work, and cancel this program.
Dr, kamal deyab mohamed -MD-ND-BCNP October 12, 2010
very impressive , may God bless you —temple of God on earth ——yours in faith , healing ,compassion care and LOVE ( THE UTMOST HIGHEST VIBRATION IN THIS EXISTENSE …. KAMAL 214-664-6044 — 2406 SYRACUSE DRIVE – IRVING – TEXAS 75062 —–drkamaldiab4@ymail.com
David October 13, 2010
Tim,
You have lost focus for the goal of medicine, it is to cure the patients of their ailments regardless of the drug, or technique, science based or anecdotal. I am all for whatever methods can provide relief for those who are suffering, regardless how “scientific” the approach.
Dr. Walshen
Martin October 13, 2010
The problem with alternative medicine is it drives people who are ignorant into the arms of those who will take their money and give them nothing in return. Instead of receiving treatments that could save their lives they may just die. All this is doing is exploiting the placebo effect.
Catherine Arnott Smith October 13, 2010
Unfortunately, this article has some definitional issues and conceptual leaps that don’t make this important and necessary conversation any easier. Alternative, complementary, and integrative medicine are not synonymous but represent different stages along the evolutionary continuum described here. “Allopathic” medicine was a label originated by homeopaths to describe their philosophical opponents, but is not really a synonym for orthodox medicine, nor is “Western” medicine (homeopathy, for example, was promulgated by a German). Statements like “There is now ‘good evidence for acupuncture'” are insufficiently detailed — would we accept a conventionally oriented physician’s statement that “There is good evidence for surgery?” Good evidence for surgery doing what, exactly? Yes, there is good evidence for some things and not for others. I’m in favor of increased access to evidence-based information about these therapies, because it will let patients make informed decisions. The Cochrane Library, available remotely to people affiliated with the UW, is a good place to start. Check it out at http://ebling.library.wisc.edu/.
Hollis Moore October 13, 2010
I find it strange and quite sad that part of what makes this “alternative” practice’s approach successful is that the doctors spend enough time with their patients to understand their concerns and start to consider the etiology as well as the symptoms. I hope that one day our health care system will have evolved to a point where doctors being able to give their patients sufficient time and consideration to help them promote their own short-term and long-term health is not the alternative, it is the norm.
Leslie October 13, 2010
I would like to speak only on Acupuncture. The fact remains, whether people “believe in it” or not, that more people have been treated with acupuncture over 5000 years than with any other form of medicine. It is not “extinct” medicine but is still continuing to help individuals all over the world.
It is “real medicine”.
In the United States, Acupuncture is state-licensed, regulated mostly by medical boards (yes, “orthodox” medical boards) and supervised by state acupuncture advisory committees, comprised of both licensed acupuncturists and physicians. (I hold acupuncture licenses in three states and have facilitated licensing in the fourth).
Acupuncture and Asian Medicine is now, additionally, taught at many well-respected medical schools across this country to enrich their “orthodox” medical education.
The goal here is not “either/or”. The goal is integrating different modalities to help patients to heal. The idea is to be as resourceful as possible to offer a comprehensive program for patients.
If you hold that acupuncture is not a form of medicine complementary to “real/conventional/orthodox medicine”, then perhaps you might update yourself on the “evolutionary continuum”.
For myself, I would be honored to work in this exciting and integrative program.
Bradley October 14, 2010
I spent twenty years seeing “real/conventional/orthodox” medicine specialists and none of them could identify the problem and instead only tried to treat the many symptoms. One visit with Dr. Rakel was all it took. No medication no extra visits needed. A drastic change in diet has greatly improved my condition. Thank you Dr. Rakel you are an extremely knowledgeable and very compassionate doctor. Thank you for looking at the whole picture and identifying the problem rather than treating symptoms.
Bradley
Steve October 14, 2010
No, acupuncture is not “real medicine” – it is not based in science. We haven’t got a scrap of evidence supporting theories of meridians or chi. Like Dr. Walshen, I’m all for anything that relieves suffering, whether “scientific” or not, but please, let’s have physicians practicing science-based medicine and leave the rest to the mystics and gurus.
Will October 14, 2010
Tim’s comment sums this up pretty well. I was shocked and a bit disappointed to see this on the front page. There is a clear line between real medicine and fake medicine, and fuzzing the boundary is neither ethical nor efficient.
Let’s start with acupuncture. First of all, it does not work. Numerous studies (placebo controlled by the way, not “he poked me and my hiccups went away! Magic!”) have concluded that the location of the puncture, the type of needle, and just about every other medically relevant aspect of acupuncture treatment makes no difference in outcomes. What does make a difference? What the patient is being told will happen, what the setting is like, who the doctor is, etc. In other words, its all psychological. There isn’t even any controversy over this except on the fringes of the medical profession, unlike over other CAM treatments such as meditation and guided visualization, the efficacy of which have not been established.
Furthermore, the very basis of acupuncture, meridians of energy running through the body, simply has no evidential basis and makes no sense given our knowledge of biology and the universe in general. There is legitimate knowledge left to be gained about medicine, and some of it will come from the alternative medicine community. But we’re not going to find it by playing fast and loose with science and believing what feels right to use instead of subject our beliefs the close and rigorous scrutiny.
Kim October 14, 2010
Tim,
Have you read Dr. Rakel’s books? His work is based on solid evidence. Plenty of double blind studies referenced in his books support the therapies he discusses. Do your homework. Don’t stay stuck in narrow orthodoxy.
Dan October 14, 2010
Met Dr. Rakel once for my chronic back pain and found him actually interested in me as a person. We spoke for a while and he made some suggestions in changing the patterns he thought were causing my back pain. I followed his advice and though I will never be totally pain free, I am now off pain meds that I took for over five years. I consider him a kind man that gently guides you to help yourself.
The one problem with the strictly scientific approach to healing is that it often leaves out the whole person. Alternative medicine is another tool in the tool kit. For some it will work, for some it will not. For me, it has helped where pure science failed.
Dr. Rakel, let me know if you ever open up for new patients, I will be the first in line.
Dale October 15, 2010
Your conversion to “integrative medicine” was inevitable as it is for anyone in a medical discipline IF they are open to looking beyond the drug-based disease model of medicine to a preventative health maintenance model. The integrative approach could be so much more cost-effective, BUT would not rake in the billions of dollars to insurance stockholders who often spend less than 20% of their premium intake for the care of those who pay the premiums. I encourage you to also look at Music Therapy as it is based on very sound scientific data, now increasingly focused on the effects of music on brain functions, and is used very effectively in obstetrics, oncology, surgery, hemodialysis, pediatrics, neurology, immunology, psychiatry, and for treating autism, aphasia, dementia, and a wide variety of developmental disabilities.
Brenda Dottl RN BSN October 17, 2010
I am very pleased to see this article in On Wisconsin. It shows how insightful and forward thinking the UW continues to be. Integrative medicine is very important, vital to the future of Health care in the US.
According to the World Health Organization, the United States ranks 37th in overall health.
http://www.photius.com/rankings/healthranks.html
In the US, we excel in Acute care, we have the best technology and resources at our finger tips, yet we have embarrassing long term and infant mortality statistics.
Our doctors are trained to depend on lab and diagnostic tests, which are not good for early detection. We don’t diagnose cancer until it’s large enough for surgery, chemo or radiation.
Our medical system is designed to profit when we are ill. (think about it).
We treat nearly everything with a chemical or surgery. We are losing sight of the Art of Medicine. As Americans, we can no longer afford to not investigate Alternative, Complementary, or Integrative medicine.
As Americans we need to look at the long term consequences of our behaviors, and we need a health care system that truly teaches us signs and symptoms of the beginnings of ill health so we can stop the progression of disease and debility. We need drugs to treat the acute problem and simultaneously the information on how to treat the cause of the dysfunction.
I have been a practicing RN for 24 years. Weekly, my patients tell me, “my tests came out fine, and everyone tells me I’m doing well,so why do I feel so bad?”
Most of my patients are taking between 15 and 30 Pills a day.
I love being a nurse, but it is sickening me that in our society we diagnose people with chronic diseases, tell them they will be on drugs for the rest of their lives, and watch them slowly die for the next 5-15 years believing there is no cure. This is not good medicine. The most difficult part for me, is knowing that chronic diseases are increasing, and they are occuring earlier in our lifespan. Life expectancy is starting to decline.
The good news, is that there is a lot that can be done for the future of Health Care and Dr. Rakel is part of the Answer.
Brenda Dottl RN
Mike October 17, 2010
I personally am all in favor of any medicine that carries no negative side effects. Especially if it is all natural. But one thing I disagree with Dr. Rakel is that I’m not very much into imagery medicine. I think that with medicine it is important to focus on the body, the organs, the overall energy, the posture, nutrition, knowledge, that kind of stuff. I even read that british MD’s in the 1920s visually confirmed the existence of hairlike mini-nerves in the exact same places that the chinese have theorized the meridians to be. Think about that the next time you are considering going under the knife! If meridians are real, then surgery is a very bad idea and should be avoided at all costs. Act early, heal better. And I don’t need to go into detail about what everybody already knows: most pharmaceutical drugs are actually worse than placebos.
On a personal note, I must say that I was fortunate enough to get to see Dr. Rakel when I was an undergraduate, and discuss some very challenging chronic disease diagnoses I had been dealing with already for over ten years. Needless to say he inspired me greatly.
Bravo Dr. David Rakel, and bravo to the University of Wisconsin for recognizing the salience of non-invasive and non-damaging therapeutics.
Mark October 18, 2010
Tim is right.
Why should people touch each other or peacefully meditate to keep from becoming too stressed when they could just take drugs to make them feel better? Besides, if people didn’t need to buy as many drugs, it would really be unfortunate for pharmaceutical companies, and of course the economy at large.
We cannot let these “alternatives” threaten us. We must stay strong and resist all that is unfamiliar. We need more evidence to show that human touch is a good thing. I prefer not to be touched at all, and I am still alive. Why can’t people be normal and just take a bunch of drugs?
Melissa October 18, 2010
I think it is ignorant to simply discredit “alternative” practices just because the science behind them has not been proven yet. Just because we cannot scientifically explain why something such as acupuncture works, does not mean that there is not a scientific process behind it. We are far from understanding all of the intricacies of the human body and its healing processes. It is silly to say that just because something cannot be explained it is not worthwhile treatment.
Personally, I have dealt with on ongoing illness for the past 8 years and have been to upwards of 7 different specialists and been on 10 different medications that have come with scores of different side effects, some of which were so severe that they put my life on hold completely. This is not answer to curing a disease. These medications and treatments focused on a singular part of my health and instead of working with my body to heal itself they were in a constant battle with what my body was naturally trying to do. I think one of the biggest benefits of many alternative treatments is the fact that they work with your body and the natural processes that are already taking place. Its not a battle between synthetically produced reactions and natural processes but rather inducing natural processes that your body needs to heal itself.
How can this not be the better option for patients? I am a proponent of “orthodox” treatments when they are needed but if alternative practices are offering less invasive and harsh options that can solve a patient’s needs, why not? Even if we cannot explain why it works.
As for my own illness, it has practically vanished in a matter of 3 months since beginning treatment with an acupuncturist. As a med student I cannot explain to you why this treatment has worked but I can certainly attest to its effectiveness, and I cannot ignore the life changing benefits it has had for me.
Pam Pappas MD October 25, 2010
Bravo to Dr. Rakel for practicing in, and trying to enlighten, such a conservative (and in some cases ignorant) area of the country.
I’m sure he will help many patients — who would otherwise be doomed to “medicine as usual” these days. By this I mean being rushed through their appointment times, dutifully drugged as most of us are taught from first year of medical school on, and ignored as unique human beings who have powerful healing resources within which can be accessed, stimulated, and strengthened.
Please keep us posted, Dr. Rakel. I am glad to call you my colleague.
Sincerely,
Pam Pappas MD
Tim October 29, 2010
To be clear, my comment had nothing to do with the general issues of whether it is better to use more or less invasive approaches (obviously, the less invasive the better, and I am not in favor of peddling pills over other accepted courses of treatment) or whether it is better to spend enough time with patients to ensure a proper diagnosis (clearly it is). These are red herrings. My point is that we need to ensure that there is a solid basis for any medical intervention. The human brain is prone to all kinds of irrational processes, and the best way to ensure we are not wrongly influenced by them is to subject our theories to the scientific process. It surprises (and scares) me to see the comments of doctors and nurses in particular who do not seem to recognize this.
If we promote the kind of thinking advocated in this article, people will continue to believe that acupuncture or other false therapies can be used in place of conventional medicine (note one of the comments above for a good example of this). We can already see the influence that such lax thinking has brought in terms of reducing the number of people seeking vaccinations. How can the University of Wisconsin teach its students to rely on the scientific method when part of the University is pushing treatments that fail this method?
Natalie November 2, 2010
To those of you bashing alternative medicine, please educate yourself more on it first. It is a little pathetic to be ashamed of UW for this. It is called “integrative” for a reason. It is looking at a patient as a whole person and not just their disease (some people actually like that!). It is great to have your own opinion; but to be embarrassed for something that has brought life back to so many people, that’s what you should be ashamed for. If the therapies work for people, then they are not “false” therapies. We can spend all the time we want defining the word “medicine” or we can do something about it and help patients to their greatest potential by complimenting our own “Western Medicine” with alternative therapies. Dr. Rakel is doing a wonderful thing that has inspired so many! I am deeply sorry you have not had the chance to experience that.
Emily November 2, 2010
I’m a recently certified family nurse practitioner and throughout this article I kept thinking “That’s what I learned!” Throughout my nursing career I have been taught to treat the patient, not just the disease. Keep up the great work, UW! And, if you need an FNP, let me know!
Dawn October 7, 2011
Keep up the good work Dr. Rakel. I am glad to see UW Health get an Integrated doctor like you. I wish I had a choice to see a doctor like you, but can’t because of Insurance not covering it. Scientific or not, if it works, that’s all that matters. I am only 48 years old and have suffered over 20 years with Fibromyalgia, Chronic Fatigue Syndrome, Chronic Pain, Chronic Headaches, Muscle Pain, Weakness, Insomnia, Stress, Anxiety, and Depression. I also have Degenerating Spine, Ruptured Spinal Disks, Nerve Pain, Arthritis, and the list goes on. Two years ago, at 46 years old, I went into cardiac arrest because of 2 blocked arteries and a 3rd one partially blocked. I’m sure it won’t be long before that one is totally blocked. I was diagnosed with Heart Disease, High Blood Pressure, Sleep Apnea, High Cholesterol, Pre-Diabetes, & low Vitamin D. I have seen too many doctors to count and have been on about 100 different medications. If one didn’t work they would give you another, and another, and another. Many meds were new with a lot of side effects, some maybe long term. Most doctors would rather give you meds instead of alternative ways. There is also conflict of interest as some doctors have financial relationships with pharmaceutical companies and that makes me even more uncomfortable taking meds. I’m only on 6 meds now, after recently stopping 3 more of them. I believe most of my health problems could have been less disabling, less painful, and some even prevented if I could have seen an Alternative or Integrated doctor. I can’t wait for the day my Insurance will pay for one of these fantastic doctors instead of paying MANY THOUSANDS of dollars a month for pills. Maybe then I can have a little bit of a joy in my life with my 2 year old grand-daughter and family. As of now, I am imprisoned in an unhealthy body of pain, fatigue, and misery.
JANET December 15, 2011
i HAVE WORKED IN HEALTH CARE FOR 35 YEARS AND HAVE SPENT 20 OF THOSE YEARS STUDYING HEALING TOUCH, MASSAGE AND HERBAL MEDICINE.I WOULD LIKE YOUR ADVISE IN STARTING A DEPARTMENT OF COMPLEMENTARY THERAPIES HERE WHERE I WORK. THE PERSON IN CHARGE SAID” HOW WILL IT WORK. HOW WILL IT START?” GIVE ME A HINT HOW YOU STARTED.CAN PEOPLE FROM OTHER HOSPITALS HAVE ACCESS TO YOUR POLICIES AND PROCEDURES FOR THIS?
GramE August 9, 2012
I don’t know that you will ever see this, but thank you, Dr David Rakel. I belong to a group of 40 or so women with CRPS. I can tell you that calming women who have been to see their PCP, their PT, to the ER, etc, etc, is a big part of what we do as a group. It is heartening to have a you woman see a new physician and come back excited to have been there. The best response, but sadly not often heard, is that “they listened and heard what I was saying”. Not even necessary to add and provided me with a miracle cure! The miracle is that a physician has taken time to listen, hear and agreed to come alongside and help me on this journey through my pain. Most often posts after appointments are filled with pain, anxiety and hopelessness. Many women comment that they learn more from other women with great Drs than they do from their own physicians. A new woman joined this week, and stated she has learned more in a week than in 13 yrs of medical treatment, but I think the reason for that is that we are willing to hear what she is saying and accept it at face value and tell her honestly that she can live within the boundaries her body has now set for her. Her sad tales of treatment are the same ones we hear over and over. So again I say, thank you for what you are doing to instruct new Drs on how important bedside manner and listening skills are to the well being (and retention of) their patients. God bless you. Ps. I do have a Neurologist who wants me to live as full a life as possible with as few chemicals as needed! And he’s not afraid of putting his hand on my shoulder and saying, “I want to help you” when my pain has gotten the better of me. But I don’t have a family Dr or an Internist who will treat me from the perspective of how CRPS affects everything I do. Still searching. Wish I lived in Wi after learning of your practice!
Kris August 21, 2013
I find it difficult to support the concept that a single provider, trained in medicine, should provide clinical care in areas for which specific providers are available. For example, there are physical and occupational therapists, registered dietitians-nutritionists, and certified acupuncturists to whom patients should be referred if they would benefit from such therapy. These providers stay on top of their literature and some are also involved in clinical research related to their care. Patients should expect that evidence-based medicine at UW Health – whether “alternative” or “traditional” – is practiced by all providers. Akin to the adage, “it takes a village to raise a child,” patients should have access to the full plethora of qualified and specifically-trained providers with the UW Health system. In other words, in our new health paradigm, perhaps it takes a team to provide optimal, holistic, patient-centered care.