Separation Surgeon

Before their separation, twins Angelica and Angelina Sabuco had become adept at toddling sideways together, but their combined weight of 55 pounds was troublesome for their mother, who had to lift them at times. Courtesy of Lucile Packard Children’s Hospital
Doctor Gary Hartman has become a world expert in the esoteric specialty of conjoined twins.
It’s November 1, 2011, at Lucile Packard Children’s Hospital at Stanford University, and pediatric surgeon Gary Hartman ’70, MD’74 is patiently and meticulously separating the fused livers of two-year-old conjoined twins Angelina and Angelica Sabuco, who were born linked from sternum to navel. He is a calm and steady presence in a scrum of a dozen surgeons, anesthesiologists, and nurses.
A sign on the operating room wall says in large letters: “Ina Red, Ica Blue” — a reminder to the team of which pint-sized, nearly identical patient is which.
Through careful planning, consummate skill, and the use of new, high-tech equipment, Hartman manages to avoid interrupting the blood flow to the two livers, a potentially fatal outcome because two blood vessels within the livers crossed over from one twin to another.
But several hours into the surgery, another obstacle looms: will surgeons be able to close the girls’ gaping wounds?
“The defect was huge,” says Peter Lorenz, a pediatric plastic and reconstructive surgeon who partnered with Hartman on the surgery. “It was basically an oval window from the neck to the belly button.”
Lorenz and Hartman turn the now-separated sisters onto their backs, and Angelica is moved to an adjacent room. For most of the next three hours, they reconstruct Angelina’s torso while another pediatric surgeon/plastic surgeon team focuses on Angelica. The teams don’t know at first if the sisters have enough extra skin — produced by tissue expanders placed in two spots under each girl’s skin in the months before surgery — to close the wound. If not, the twins could die from infection, a not uncommon occurrence in such separations.
“We used every bit of real estate we could for tissue,” Hartman says. As it turned out, the expanders worked — they just barely managed to do the job, with no skin to spare.
Within seventy-two hours after the ten-hour surgery, Angelina and Angelica were breathing on their own. After six days in the hospital’s pediatric intensive care unit and another seven in the hospital, they were strong enough to go home. They have since had follow-up visits with plastic surgery and physical therapy to learn to walk straight ahead and develop their gross- and fine-motor skills.
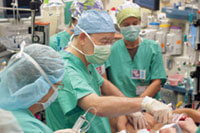
Pediatric surgeon Gary Hartman (center) is used to performing complex procedures that have all the intensity of a NASA space mission. Courtesy of Lucile Packard Children’s Hospital.
The Sabuco separation was Hartman’s fourth as lead surgeon and his sixth separation of conjoined twins overall. Hartman, who has been at Lucile Packard since 2004, is believed to have participated in more separations than any other pediatric surgeon in the world.
The frequency of conjoined births is hard to pin down, Hartman says, because so many of the twins die in childbirth or soon after, but estimates range from 1 in 50,000 to 1 in 100,000, with an overall survival rate of about 25 percent. Separation of such twins is one of the rarest types of surgery; only about six separations are performed each year in the United States, and few pediatric surgeons ever encounter the condition.
While procedures such as the Sabuco twin separation have brought Hartman international attention, he has performed even more complex pediatric surgeries. His most complicated cases involve correcting birth defects and removing tumors. He has fixed such things as a blockage of the esophagus or the absence of an anus at birth. One eighteen-hour surgery, Hartman’s longest, corrected a baby’s tangle of abnormal blood vessels around the neck and chest.
What every procedure has in common, however, is the goal of saving or improving the lives of children who have been dealt a bad hand. “Pediatric surgery is a combination of the routine and the extremely rare and devastating,” he says, noting that to him, the routine cases are just as important as the complex ones. “Kids with appendicitis, they’re hurting and sick, so when you send them home in good shape, that’s rewarding, too.
“Children don’t cause their illnesses — they’re victims of it,” Hartman says. “They’re so honest. When they’re upset, it’s clear, but they’re very forgiving. They’re a nice population to work with.”
The Sabuco surgery had the intensity of a NASA space mission. The culmination of nearly a year of planning, it was carried out by a team of almost fifty doctors, nurses, and operating-room staff. Two weeks later, the active, dark-eyed girls from the Philippines — now living in San Jose, California, with their parents and older brother — left the hospital wearing matching bright red dresses and, for the first time, riding in separate car seats. Today, they are catching up with their peers in every developmental marker.
Their lives could have turned out much differently. Angelina and Angelica had what is called a thoraco-omphalopagus connection, with separate hearts, brains, kidneys, stomachs, and intestines. YouTube videos of the girls before their operation show how adept they were at toddling sideways together. But their combined weight of fifty-five pounds was proving troublesome for their mother, who had to lift them at times. Their spines were being distorted by their connection at the breastbone, and their lives as individuals — they were already showing personality differences, with Angelica the more outgoing, aggressive twin — would have been drastically circumscribed without surgery.
The Sabucos originally sought out Hartman after an Internet search of conjoined-twin specialists kept turning up his name. At a press conference after her daughters’ successful surgery, a tearful Ginady Sabuco thanked Hartman and his colleagues, saying, “This is a dream come true. … My family will be grateful eternally.”

Hartman’s MBA comes in handy when he engages in the extensive planning required for operations that can involve up to 100 people. Courtesy of Lucile Packard Children’s Hospital.
Hartman’s journey to Stanford started in Wisconsin Rapids, where his parents owned and operated the local furniture store. He became interested in psychology in high school, enrolled in the College of St. Thomas in St. Paul, Minnesota, and transferred as a sophomore to the UW. “I went from two thousand Catholic boys at St. Thomas to thirty-eight thousand maniacs in Madison,” he says. “But between my meal job [serving lunch and dinner at a private girls’ dorm in exchange for meals] and classes and classmates, it didn’t feel that big — it felt very comfortable and nurturing.”
After earning his bachelor’s in psychology, Hartman says he naively applied only to the UW for his medical training. “It was stupid — I didn’t know how competitive things were. But I wanted to go to UW medical school anyway, because it was a great med school, and for in-state students, a really good deal.”
Hartman says he’s particularly grateful for encountering a medical pioneer at the UW, Helen Dickie, a pulmonologist and professor who mentored thousands of Wisconsin students from 1955 until her death in 1988. “She was probably the toughest professor I had,” he says. Dickie had amassed a library of hundreds of x-rays she used during her teaching rounds: “She would throw up x-ray after x-ray, and you would fumble though reading them and making a diagnosis. She really put her medical students on the hot seat, but I think I learned the most from those sessions.”
After graduation, Hartman did his internship and general surgical residency at Highland General Hospital in Oakland, California, rotating to most of the hospitals in the San Francisco Bay Area. He found his specialty during a surgical rotation at Children’s Hospital in Oakland in the mid-1970s.
“I became enamored with pediatric surgery because of the spectrum of conditions, the delicacy of surgery, and just dealing with kids,” Hartman says.
Hartman earned an MBA from George Washington University while working at Children’s National Medical Center in Washington, D.C., and is known for his businesslike preparation before complex procedures.
“Gary is one of the world’s experts in pediatric surgery,” says his colleague Thomas Krummel, surgeon-in-chief at Packard Children’s Hospital. “He has brought real twenty-first-century planning to what are incredibly complicated operations, some involving fifty to one hundred people.”
Only two dozen or so medical personnel can be admitted to an operating room at any one time, so if a surgery takes more than twelve hours, a second shift of staffers is required. Planning and executing these risky procedures also calls for help from numerous administrative and support staff.
With so many bodies jockeying for position during a surgery, preparation is key, Hartman says, so the team plots the position of every staffer and instrument beforehand on a detailed diagram. “Then we do live mock-ups where we go into the operating room in the evening, bring in all the instruments, and turn them on,” he says.
Hartman performed his first conjoined twin separation in 1982 during a fellowship at the University of Oklahoma. He was the lead surgeon on his fourth twin-separation surgery at Children’s National Medical Center in 2004 when Hartman and his team encountered a nasty surprise during a rehearsal: when all the surgical instruments were plugged in, the power failed. “We had to drop additional power into the room,” he says.
In 2007, when Hartman performed his first separation at the Stanford children’s hospital — and fifth overall — the hospital upgraded an existing operating room. By the time the Sabucos were operated on, the hospital had a room specially built to accommodate the surgery and its legions of instruments and personnel.
The late-in-life adoptive father of a thirteen-year-old girl — “It’s a challenge,” he says happily about raising a teenager with his wife, Susan — doesn’t stop seeing his young patients after they’ve left surgery. “That’s the best part,” he says about monitoring the progress of the Sabuco girls as they receive therapy at the hospital to help them adjust to life as separate individuals. “Last time I saw them, they were running up and down the hall, one going one way and one the other way. They look like normal girls — very sweet, loving, and attentive of each other and their family.”
Although the twins’ surgical wounds have healed, Hartman will continue to see Angelina and Angelica for years to come as he follows the growth of their chests and breastbones.
The rewards of his chosen specialty literally last a lifetime, Hartman says. “If an adult surgeon does something fantastic with a 50- or 60-year-old, the patient may live another twenty or 30 years.
“If we get things right with a baby, that child will get 70 or 80 years of use out of what we’ve done.”
Melissa Payton is a freelance writer and editor in Portland, Oregon.
Published in the Summer 2012 issue



Comments
Joanne8777 June 6, 2012
Dr. Hartman is one of the kindest, most sensitive and intelligent men I’ve ever met. These wonderful qualities are an asset in his work, which requires incredible attention to detail, patience and fortitude.
Thank you for a wonderful article! I really enjoyed reading it!
Nicholas E. Couse, D.D.S. June 19, 2012
Congratulations, Gary, on a very successful career! Nick Couse
Classmate of Al Hartman AHS 1963