Listening to Typhoid Mary
Can we stop untreatable infections without stomping on civil liberties?
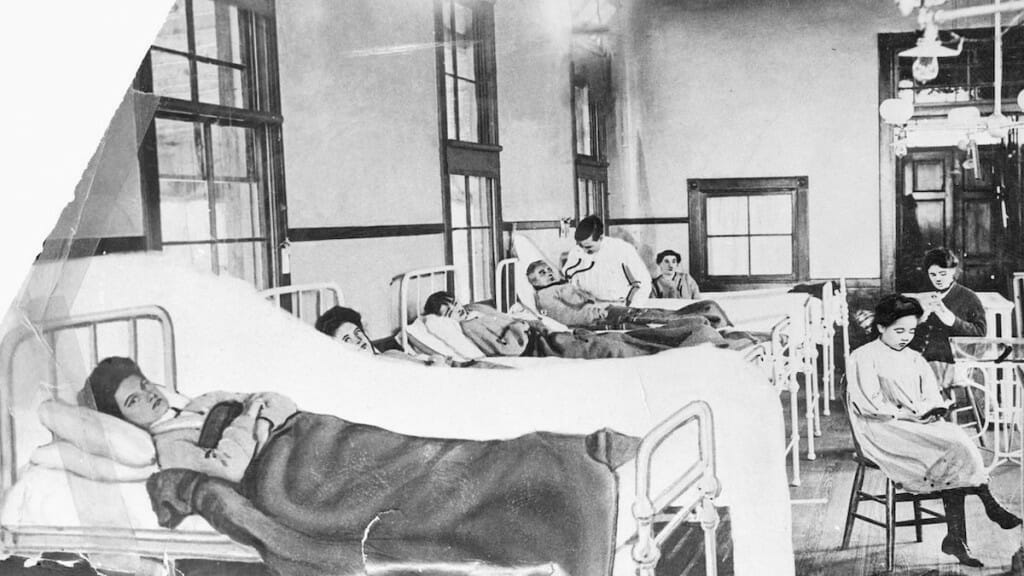
Irish immigrant Mary Mallon, seen in a New York hospital bed shortly after she was seized by public health officials in 1907. Bettmann/Corbis
Editor’s note (March 17, 2020): This story was first published in the Winter 2004 issue of On Wisconsin, following the SARS outbreak. We are republishing it in full, as it contains relevant historical information as society grapples with the COVID-19 pandemic.
Multiple-choice test: What stopped the spread of deadly SARS in 2003? Was it (a) modern science, or (b) ancient practice? If you guessed (a), guess again. Modern medicine has learned a lot about the virus that causes severe acute respiratory syndrome, but it offers neither prevention nor cure.
Instead, credit the ancient practices of quarantine and isolation for containing SARS in its place of origin, China, as well as in a related outbreak in Toronto, Canada. The epidemic, which infected 8,098 people around the world and killed 774, could have been much worse without the simple measure of separating the sick from the healthy.
But while they may be medically effective, isolation (which refers to the separation of people with active cases of an infectious disease) and quarantine (which isolates those who have had contact with active cases) involve deeper tensions between public health and individual liberty. With quarantines in particular — when public-health officials wield power to segregate people who may be perfectly healthy — it raises a thorny question: Am I willing to put up with limits to my freedom to keep you safe from infectious diseases?
For Mary Mallon, the Irish-born cook who helped trigger an outbreak of typhoid fever in New York City in the early 1900s, the answer was no. Although she never contracted typhoid herself, Mallon was a healthy carrier of the intestinal bacterium that causes the potentially deadly illness. After she was blamed for spreading the fever through food she handled in her employers’ kitchens, she was dubbed Typhoid Mary, a name that has come to signify anyone who jeopardizes the public health by carrying and transmitting disease.
Mallon’s fate has long fascinated Judith Leavitt, a professor of the history of medicine at UW-Madison. “I am convinced that until the day she died, she was not convinced that she was a danger,” says Leavitt. In her view, the fact that Mallon felt no symptoms of illness and never understood why she was barred from human contact illustrates the fundamental conundrum of quarantine. “She was healthy; no way could she believe she could transmit typhoid,” Leavitt says.

Mallon was forced to live in this tiny house on an island in the East River for nearly thirty years. New York Municipal Archives
Forward to the Past
Not long after 1938, when Mallon died in isolation, the importance of quarantines seemed to fade as vaccinations and antibiotics put microbes on the run. From the end of World War II until the appearance of AIDS around 1980, infectious disease seemed destined to be more history than science. “We thought we’d conquered infectious disease,” says Leavitt.
Hardly. HIV, the AIDS virus, joined a frightening run of new and resurgent pathogens that included Legionnaires’ disease, a respiratory infection that grew in air ducts; Ebola, an African bleeding disease; hantavirus, carried by rodents in the American Southwest; and Lyme disease, spread by deer ticks across the Northeast and Wisconsin. Biologists learned that bacteria can develop and share genes that make them immune to the “wonder drugs” designed to kill them. Many old microbes, such as influenza and tuberculosis, have resurfaced in new, super-resistant forms.
Some diseases, including influenzas, can jump between species in an unending cat-and-mouse game with animal immune systems. Many human influenzas originated as a virus in birds, which explains the intense concern sparked by a flu that is scourging poultry in Southeast Asia. The virus — and deliberate extermination of infected flocks — have killed 100 million fowl in just two years. Until recently, every human case of that bird flu was traceable to contact with fowl. But in September, Thai authorities began investigating possible cases of human-to-human transmission — an event that could allow the flu to travel far beyond the flocks where it currently is contained.
In a reminder of the killing potency of influenza, UW-Madison virologist Yoshihiro Kawaoka recently demonstrated that only a few genetic tweaks separate mild forms of flu from the lethal virus responsible for the global flu pandemic of 1918–19, which claimed 20 million lives. Add in the fragility of the systems we have to fight the virus — as powerfully demonstrated by the flu-shot crisis in which contamination wiped out roughly half of the U.S. supply of vaccine — and you understand the growing dread among many scientists of another pandemic.
But our renewed concern about infectious diseases did not stem just from the natural evolution of microbes, nor from their increased mobility through globe-hopping jet planes. The anthrax attacks that killed five Americans in 2001 raised the threat of biological weapons to a nation already traumatized by the September 11 attacks. While the Iraqi bio-weapons threat proved illusory, it’s now clear that a massive Soviet program spent decades brewing weapons from a smorgasbord of deadly microbes. Although it would be difficult to pull off, an expert attack using drug-resistant microbes, alone or in combination, could start a pandemic.
That reality has public-health officials scrambling for antidotes, and quarantine, one of the oldest tools in the bag, may also be one of the most reliable against these threats. According to a report published in January by the Centers for Disease Control, “SARS provided an example of the power of traditional public-health measures — including surveillance, infection control, isolation, and quarantine — to contain and control an outbreak.”
Quarantine, in fact, vastly predates the discovery of microbes. In 549 A.D., the Roman emperor Justinian tried to stop bubonic plague by isolating the sick. China also quarantined plague-stricken sailors returning from the sea during the seventh century. The effort to contain pathogens continued through leper colonies and tuberculosis sanatoriums. As people congregated in ever-larger cities, quarantines became the province of public-health departments that arose to control the rapid spread of diseases in crowded urban areas.
The poster child of quarantine remains Mary Mallon, who was twenty two years old in 1907, when she was identified as the source of a fearsome typhoid fever outbreak in New York City. Blaming six cases of infection on her, public health authorities shipped her to an island in the East River, where she spent three years before being released on the promise not to resume cooking. In 1915, however, she was caught working under a pseudonym in the kitchen of a hospital where twenty-five people had contracted typhoid. The health department returned her to the island, where she lived, solitary and bitter, until her death.
Mary, Mary, Quite Contrary
Although Mallon furiously resisted her imprisonment, she attracted little sympathy from a public more concerned about its health than her liberty. She was, in a sense, a prisoner who neither understood her crime nor repented it. A letter Mallon wrote in 1909 gives a flavor of her attitude: “There was never any effort by the Board [of Health] authority to do anything for me excepting to cast me on the island and keep me a prisoner without being sick nor needing medical treatment.”
You could see the Mallon story as a simple triumph of public health over a willful, ignorant, infectious immigrant. But for Leavitt, whose 1996 book Typhoid Mary: Captive to the Public’s Health was the basis for an episode of Nova aired in October, it’s not so simple. She believes that public-health authorities were more eager to prove their power than to help Mallon understand her situation or find a safe way to make a living.
“I am convinced she was a healthy carrier, and if she cooked for people, she had potential for infecting them. But there were a lot of things she could have done that were perfectly safe,” Leavitt says. Although the idea of retraining arose during Mallon’s second quarantine, by then, Leavitt says, “she’d developed a pretty strong resistance” to advice from the health department.
Did her case reflect pure injustice or pure medical necessity? “I think it’s somewhere in the middle,” says Leavitt. “It was certainly not only an injustice.”
The tensions in Mallon’s case have echoed through the history of quarantine and isolation, says Richard Keller, an assistant professor of medical history and bioethics. In the 1930s, for example, in the French colony of Tunisia, the eminent bacteriologist Charles Nicolle was in charge of controlling epidemics. Nicolle had already won the 1928 Nobel Prize for identifying lice as the carrier of typhus in Tunisia. “When bubonic plague broke out in 1930,” says Keller, “he initially suspected that it was a migrant-laborer population that transmitted it, so he rounded up four hundred soldiers, sent them to buildings where the migrants were living, took them to a prison, and quarantined them.
“What was so remarkable was that there was only one case of plague, and the source was elsewhere,” says Keller. “But this guy was director of the Pasteur Institute, had won the Nobel Prize, [and so] he must know how diseases operate. Yet he couldn’t think beyond the idea that a given population must bear responsibility. It’s a frightening aspect of how science and public health often interact.”
Discrimination and instinctive blaming were also evident, Keller argues, in the early 1980s, at the start of the AIDS epidemic. Haitians, he says, were singled out as a source of infection, even though other subgroups had a higher rate of HIV infection. “Haitians were the only population, on the basis of ethnicity, that were banned from donating blood,” he notes.
Taking It to the Streets
If there is one thing we know about controlling epidemics, it is that the behavior of the public matters. Whether you’re trying to keep the sick at home or get immunizations to the uninfected, you must enlist the cooperation of the community. But the actions of public-health authorities can do as much to antagonize the public as to reassure it.
As an example, Leavitt contrasts an 1894 smallpox vaccination campaign in Milwaukee with a similar effort undertaken in 1947 in New York City. Milwaukee’s authorities bungled the response, she says, by stressing the letter of the law and discriminating against the poor. In a 2003 article, she argued that the public health department used “strong-arm tactics on its poorer citizens,” leading to a “complete breakdown of law and order” that led to a month of rioting. As a result, the city endured what she described as a “raging epidemic,” which killed 244 citizens.
Half a century later, after a smallpox outbreak in postwar New York, an active public-health department promoted the public stake in mass vaccinations. The mayor made a big show of taking his shots, and, amid what Leavitt described as “civic order and citizen cooperation,” more than 6 million people were vaccinated in four weeks. The disease claimed two victims.
When the federal government grew worried about smallpox two years ago, it could have learned from those precedents. But the bioterror-inspired campaign to inoculate medical personnel across the country “fell flat on its face,” Leavitt says. “The public was not convinced it was a real threat. There was not enough work to be confident in the vaccine itself, nor in how the current population would respond to it,” given the large number of people with immune suppression.
“Public response matters,” she says. “A positive reaction can lead to successful programs; a negative one can prolong and exacerbate the infectious disease and put more people at risk.”
With SARS, public cooperation was a significant factor in containing it. Although the Chinese government was initially slow to act, it managed to quarantine about thirty thousand people in Beijing alone. Similarly, about seven thousand people were quarantined in Toronto, ending the Canadian outbreak. Yet as we credit quarantines for their medical efficacy, the social costs are still revealing themselves. One study published in the Journal of Emerging Infectious Diseases found that about 30 percent of people quarantined in Toronto had symptoms of post-traumatic stress disorder.
Ready or Not
For decades, state agencies charged with carrying out public-health campaigns have complained about a lack of funding and inadequate tools. Few public health departments have been able to tap into even simple technologies such as e-mail to monitor infectious diseases and disseminate information. In an age of possible bioterrorism, that is changing, says Wisconsin state epidemiologist Jeffrey Davis ’67, an adjunct professor of population health sciences at UW-Madison. Since 2001, “every state has received resources for public-health preparedness and to improve personnel and infrastructure,” Davis says. “There are more people on board doing surveillance [and] invoking plans for prevention and control, more laboratory capability to test for certain agents, and more assessments for vulnerability in certain settings.”
In Wisconsin, for example, hospitals, clinics, emergency rooms, labs, and first responders can link to a secure communications web known as the Wisconsin Health Alert Network, which is designed to speed detection of public-health threats and give authorities a way to respond quickly to new threats. “This is something we couldn’t do three years ago,” says Davis. “It’s not perfect, but every year we are more prepared than the year before.”
Such new tools are one indication that public health extends well beyond the realm of microbes and vaccines. “I would argue,” says Keller, “that public health exists simultaneously in two important domains. One we normally think of as the medical domain, but it’s at least as much in the province of law and public order.”
In that regard, we may be returning to the age of Typhoid Mary, when the hardware assembled to fight the next outbreak may matter less than the “software” — the less docile human factors that sometimes require authoritative control.
“In our country, the value of individual rights is so strong,” says Leavitt, “but so is the value of government protecting the health of people where individual efforts are not enough. You can’t expect everybody to find their own clean water, so you have a municipal water system. The same is true with some epidemic responses. There will have to be some societal response, and that will have to be coordinated by local government. Part of public health is militaristic, or at least police oriented, because you often are asking people to do things they would not think of doing on their own.”
As Davis points out, state and local health departments have always had coercive power to stop risky behavior. “If it’s serious,” he says, “a disease for which there is no effective prevention other than limiting people’s movement, and if that disease has terrible consequences, the case for quarantine can be made fairly decisively.”
But how will that fly in a nation that values privacy, liberty, and individualism? Davis is guardedly confident. “My experience, after twenty-five-plus years in the state, is that people have been pretty responsible. Given some of the things we may need to confront, I hope people will understand their responsibilities, as individuals, as people living within a family structure, and as people living in the community.”
Published in the Winter 2004 issue



Comments
No comments posted yet.