Off the Prescribed Path

Jenny Amani has generally cut her own path in life. “I guess the wiggles got the best of me,” she says. Her road has led her in and out of UW–Madison and to the Skokomish reservation in Washington. She plans to return to a residency program this summer. Photo: Rick Dahms.
Throughout her undergraduate, medical school, and professional career, Jenny Amani has never followed the usual road. Who figured the country would need to create more doctors like her?
Jenny Amani MD’09 doesn’t have many fears, but the UW School of Medicine and Public Health is one of them.
“Please be careful how you talk about me,” she says. “Medicine does not like people who fall out of line. They make a gripping Lifetime movie, but they don’t make a viable professional.”
Amani is speaking from a Native American clinic on the Skokomish reservation on Washington’s Olympic Peninsula — about as remote a location as one can find in the continental United States.
“You’ve got to see this place,” she says. “It’s a gorgeous place to practice. The Native American art is just amazing, and the people are truly thankful for your work.”
Gorgeous it may be, but it’s also something else: a refuge? a break? a self-imposed exile? It’s a departure, at any rate. It’s a fall from the straight line that doctors are supposed to follow. Amani is with the Skokomish because of the fearless decisions she’s made, including dropping out of her residency program.
She’s right — her life would make a gripping Lifetime movie, because she seldom follows the prescribed path. Her entire career, from her first undergraduate stint at UW–Madison, has avoided straight lines and instead traced curves and cul-de-sacs.
She dropped out of college.
She got involved in the club scene.
She was homeless.
She fought her way back to a degree and then to an MD.
But if she’s afraid of the disapproval of the School of Medicine and Public Health (SMPH), her fears are unfounded — she hews closer to their ideals than she thinks.
“We’re not at all embarrassed by Jenny,” says Cynthia Haq, a UW professor of family medicine. “We’re very proud of her. She’s a survivor. We’re proud of her for the difference she’s making, and of all our students who choose a career path to work with people who may not have sufficient access to health care services, the medically underserved.”
Since adding and Public Health to its name in 2005, the UW’s medical school has increased its focus on encouraging the doctors it trains to work with the medically underserved — a growing population in the United States. Though Congress passed the Patient Protection and Affordable Care Act (nicknamed Obamacare) in 2010 with the aim of providing health insurance to perhaps 30 million previously uninsured Americans, the law can’t guarantee access to health care. With or without insurance, no patient can see a doctor who isn’t there.
“Access to health care has to do with insurance schemes, but it also has to do with getting doctors and nurses to the right places, where the needs are greatest,” Haq says. “In many areas, there simply are not enough doctors to meet the minimum requirement to provide basic health care services. We need to create programs to recruit and train doctors to work with underserved populations.”
And so the UW is looking for more medical students who, like Amani, want to devote themselves to the underserved, even if the rewards — in money, in prestige — are much less than a doctor might find elsewhere. In recent years, the school has gained a reputation for these efforts. In 2013, it earned the Association of American Medical Colleges’ Spencer Foreman Award for Outstanding Community Service, naming it, in Haq’s estimation, as “one of the leading community-engaged medical schools in the country.”
Amani has been practicing on reservations for nearly two years, working with the Quinault and the Nez Perce Nations before joining the Skokomish. And she does so even though she didn’t finish her residency. She left that program when she felt she could no longer balance the needs of her newborn son with the demands of residency. Although she had passed all her exams and qualified for a state license before she left, her options were limited.
“Most hospitals and managed-care clinics require that you finish residency. But with a license in hand, you can work in several sectors. The military, corrections, and Native health are all possible options,” Amani says. “I had to start working at an occupational health clinic. I sent out hundreds of applications, and they were the only ones who would hire me at that level of training.”
But Amani, who grew up in poverty, has always been committed to caring for the disadvantaged. “That’s where my roots are,” she says. “The poor and underserved [have always] somehow found me.” When a job with tribal health popped up, she took the jump.
But then Amani’s career has seen a lot of jumping, and things have seldom gone entirely her way. She first enrolled at UW-Madison as an undergraduate in 1990, after a youth spent moving around as a military brat. But the structure of the university didn’t agree with her, and she dropped out in 1993 to pursue work as a DJ in dance clubs, first in Madison, then in Champaign, Illinois, then in Chicago.
“I guess the wiggles got the best of me,” she says.
It didn’t take her long to realize she had a naïve view of club culture. Very few patrons, she discovered, went out solely or even principally to hear her musical work. Instead, they came for hook-ups, alcohol, and drugs.
“It really came as a shock,” Amani says. “Very few people go to bars to hear music. People often ask me if I got caught up in the culture and substance abuse. But I saw what it did to people, and I decided early on that I was not going down that path. I don’t drink at all. Like, not at all. I was just spinning music and learning about life.”
Working turntables was fun, and Amani enjoyed what she calls her “urban education,” but it was hardly lucrative. Money was tight, and her parents divorced, leaving her to fend for herself. She was homeless for a time, staying in shelters, sleeping in her car, or “couch surfing” at friends’ apartments.
She saw hurt and heartache on the streets of Chicago, and she realized that she couldn’t do much to help people as a DJ.
“I always had this thought that I should become a doctor,” she says. “Even when I was spinning the tables, it was there in the back of my head. And while I didn’t seem like a likely candidate, I kept putting one foot in front of the other until I was there.”
She earned her bachelor’s degree by taking classes at community colleges and then the University of Illinois-Chicago, all the while laboring forty to fifty hours a week as she supplemented her nightclub work with a job with deaf children. After a post-baccalaureate year in biomedical sciences, Amani worked with AmeriCorps at a domestic violence shelter as she applied to medical school.
“I had to slug through it,” she says, “and I fell a lot, got sidetracked, got back on course. Many people encouraged me to keep going. I’m not particularly academically talented. I’m just the schmuck who keeps getting up every time she’s knocked down.”
Amani applied to seventy medical schools, interviewed at twelve, and was accepted by three before she stopped looking. The UW’s was one of the three, and she returned to Madison, a familiar city where she could be closer to her family.
While in school, she never lost sight of the disadvantaged. In her third year, she connected with Jim Withers, a physician in Pittsburgh who had created Operation Safety Net to practice what he calls “street medicine.”
The program puts medical professionals — Withers himself, nurses, students such as Amani — out on the street to meet with and serve the homeless on their own turf. For a semester, Amani went to street corners and alleys and doorways to do exams, give out clean socks, and connect people to the medicines they needed. She told them her own story and encouraged them to get back on their feet.
“It was a privilege to serve that way. I especially appreciated their openness, their willingness to bare the little they had,” she says. “There’s something about meeting people where they live. Whether it be a dirt pad under a bridge or a palace, they’re inviting you into them. You learn so much more about them than you can in an office.”
After graduation, she tried to keep to the standard path. She began a residency program in the Southwest, but she felt she was learning more about paperwork than patient care. Her unrest mounted during her first pregnancy, and she left her program when she felt her family priorities were compromised. After working in occupational health and general practice for a year, she found her way to the Indian Health Service.
Few ethnic groups suffer health care needs as acutely as Native American communities do. “We are perhaps the most challenged group in the country,” says Erik Brodt, a professor of family medicine and director of the UW’s Native American Center for Health Professions.
NACHP’s goal is to increase the number of Native and non-Native health professionals who work in Native communities to help solve those challenges — a very personal issue for Brodt, who is Native American. “We die younger than any other major group. We live with more chronic diseases. We have higher rates of heart disease, kidney disease, and cancer. We die more often from accidents and suicide. And I believe the paucity of health professionals and policy-makers [who are] well-educated in Native issues limits our ability to find solutions.”
But Amani feels that her career has prepared her for the challenges of working in Native health.
“It’s been a rough ride,” she says, “quite a roller coaster. But I don’t regret anything that happened to me, whether having children or leaving residency. It’s deepened me so much as a person, which has made me a better physician. I feel a deep connection to the less fortunate, and it just seems that I’m lucky enough that they seem to find me, wherever I am. The [Skokomish, Quinault, and Nez Perce have been] so appreciative of my efforts, and when they share their culture and Native medical knowledge with me, I feel so privileged to be invited into their world.”
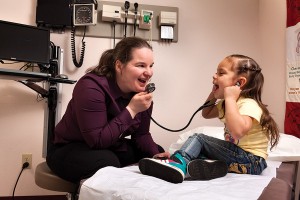
Jenny Amani treats a young patient at a clinic on Washington’s Skokomish reservation. After Amani left her residency program, the Indian Health Service was one of the few organizations that would take her. But she’s found the work fulfilling. “There’s something about meeting people where they live,” she says. “They’re inviting you into them.” P{hoto: Rick Dahms.
Amani isn’t easy to get hold of these days, and it would be a stretch to say that she’s a role model for SMPH. Few at the school even know her name. She was Jennifer Jenkins when she was a student. During her last year at the UW, she wrote about her experiences doing street medicine for an SMPH newsletter, but afterward, she largely disappeared from the school’s view.
But even if the UW hasn’t been following Amani, it’s aware that many American doctors aren’t like her, and sometimes that can be a concern. While work with the underserved has found her, it doesn’t tend to interest many physicians. A medical education is challenging, expensive, and very long. It tends to weed out all but the most driven, motivated students. As a result, some doctors can feel a bit entitled.
“Physicians are a very highly respected, high-income group,” says David Deci, a professor of family medicine and that department’s director of medical student education. “It can be easy for us to forget the struggles that the vast majority of people go through.”
Like Amani, Deci is a disciple of Jim Withers. Before joining the UW faculty in 2009, he taught at the medical school for West Virginia University, where he served as adviser to a group of students who launched their own street medicine clinic, and Deci met with Withers many times. Deci is now on the national board of directors for the Street Medicine Institute, an outgrowth of Withers’s Operation Safety Net that offers guidance to similar organizations around the globe. At the UW, he’s the faculty mentor for MEDiC, the student-run, free medical clinics that operate in a variety of locations around Madison, including several homeless shelters. (See On Wisconsin, Winter 2009.)
“The school has a mission of serving the people of Wisconsin,” Deci says. “Just as spreading research is important in giving wonderful advancements to the state and nation, we also have to serve by giving good health care to the state.”
In 2004, the Wisconsin Hospital Association and the Wisconsin Medical Society issued a report, “Who Will Care for Our Patients?,” documenting shortages of physicians across the state. It’s been updated twice since then, but the trend has been clear: the state isn’t recruiting and retaining enough physicians to care for its population.
How many is enough? The federal government defines a community as a “health professional shortage area” if there are more than 3,500 people per primary care physician (or more than 3,000 if the population includes a large portion of elderly, very young, or very poor people who require a higher level of care). By this standard, the United States as a whole is far from underserved. According to the 2010 census, there were more than 397,000 primary care doctors practicing in the country, or one for about every 800 Americans. But the physicians are far from evenly spread across the country — they tend to clump in relatively affluent areas. Wisconsin has 7,254 primary care physicians for a population of about 5.7 million, or one for every 786 citizens. And yet three-quarters of the state’s counties — rural areas and poor inner-city areas — include medically underserved populations.
In the early 2000s, the UW embraced an opportunity to expand the ways it serves the state. Blue Cross/Blue Shield United of Wisconsin converted from a nonprofit to a for-profit entity — essentially, the insurance company was sold. From the proceeds of that transaction, a sum of $630 million was to be split equally between SMPH and the Medical College of Wisconsin. From these funds, SMPH created the Wisconsin Partnership Program to serve the public health needs of Wisconsin and reduce health disparities through initiatives in education, research, and community partnerships.
In 2007, noting a decline in the number of doctors working in Wisconsin’s small towns, the UW’s medical school, with the support of the Wisconsin Partnership Program, created WARM: the Wisconsin Academy for Rural Medicine, which is under the direction of Byron Crouse. The four-year program encourages medical students to see the needs of rural areas, where the problems often stem from an aging population.
“Not only are the people in rural areas getting older,” says Crouse, “but so are their physicians. We say they’re transitioning from health care providers to health care users.”
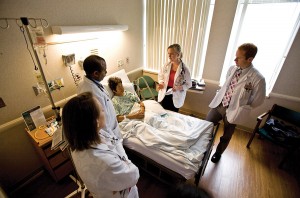
Medical students from the UW’s TRIUMPH program see a patient in this photo from 2010. TRIUMPH places students in facilities in poorer areas of Milwaukee. According to Cynthia Haq, the program’s director, participants “quickly come up against [the] reality” of what it means to practice in low-resource communities. Photo: Milwaukee Journal Sentinel.
“Many students come to work in low-resource settings with the hope that they’re going to save people, and dramatically change health outcomes in a short period of time,” says Haq. “They quickly come up against reality — for example, a forty-year-old man with mental illness who’s already had a stroke and diabetes and is homeless. These are complex problems to address, and you’re not going to be successful if you try to do it by yourself. Yet, if you’re interested in this type of work, you will find many other like-minded physicians and community members who are also contributing. You can have a rich life full of rewarding options and make a difference where the needs are greatest.”
Deci believes that the programs aren’t just good for the state; they’re good for the school and good for students. Working with the underserved, Deci argues, makes for better and even happier physicians.
“It’s so easy to be absorbed by the efficiencies and technology of modern health care,” he says. “But that can be a recipe for burnout and cynicism. When you work with the underserved, you see people’s needs holistically — biological, psychological, social, and spiritual. You spend more open-ended time with them, and because resources are often limited, they engage and challenge your skills as a physician.”
It’s that holistic treatment of patients — particularly paying attention to their social and spiritual health — that Amani finds so important in her current work, and she’d like to spread what she’s learned from the Skokomish elsewhere. She turned forty last year. Her children — two sons — are now past infancy, and she’s decided she’s ready to return to the standard path of medical education, at least for a while. This year, she and her partner, Sharon Amani, are taking their family to Texas, where she’ll start residency again at the University of Texas-Houston, doing occupational and environmental health. With this focus, she’ll earn a master of public health, which she hopes will teach her more about preventive efforts. She is confident that the poor and disenfranchised will find her in Texas, just as they did in Wisconsin and Washington.
“There’s a huge subset of the population who come to the occupational health clinics because that’s the only health care they can get,” she says. “Maybe they’re working a minimum-wage job, or maybe they don’t get health care. You try to do as much as you can for them in the moments they’re in front of you, whether that’s in the clinic, on the streets, on the reservation, or wherever you are.” n
John Allen is senior editor for On Wisconsin.
Published in the Summer 2014 issue



Comments
Wm Riley MS-88 June 15, 2014
I live 1750 miles from my Alma Mater UW-Madison, and I continue to cross paths with fellow grads like Dr Jenny
Amani. If there is a more beautiful place on the West Coast than the Olympic Penninsula, WA, I have not found it.